Meningitis Outbreak at University of Kent: Two Dead, 11 Seriously Ill and Campus Event Under Scrutiny
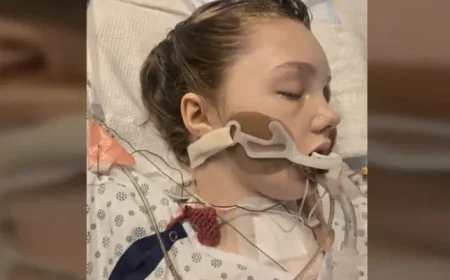
An unexpected cluster of severe illness has left two people dead, including a University of Kent student, amid a meningitis outbreak that has prompted the UK Health Security Agency to contact more than 30, 000 students, staff and their families. Authorities say 11 others from the Canterbury area are in hospital and seriously ill, most aged between 18 and 21, and that antibiotics are being arranged for some students while the specific strain remains unidentified.
Meningitis Outbreak: Background and Scope
The UK Health Security Agency mobilised a rapid response after what has been described as invasive meningococcal disease emerged in Canterbury. The agency identified multiple cases and is arranging antibiotics for people in affected campus blocks. A letter from the agency to University of Kent students and staff said people living and working in certain blocks should receive antibiotics without delay. Specialists are interviewing those affected to identify close contacts.
The cluster is thought to be linked to a social event in Canterbury that some of those who fell ill attended. Public health teams have emphasised that the specific strain of the disease has not been identified, underscoring ongoing investigation and the need for targeted prophylaxis and contact tracing.
Deep Analysis and Immediate Response
What lies beneath this meningitis outbreak is a combination of rapid progression of illness among young adults and the transmission dynamics associated with shared social environments. The UK Health Security Agency has delivered antibiotics to students in the Canterbury area and identified a cohort of people deemed close contacts; close contacts have been given antibiotics as a precautionary measure. The decision to reach more than 30, 000 students, staff and families reflects the public health judgment that a broad communication and targeted antibiotic offering are necessary to limit further spread.
Clinical descriptions provided by public health teams highlight both meningitis and septicaemia as manifestations of the invasive disease. Symptoms noted in briefings include high fever, vomiting, severe and worsening headache, rashes that do not fade under glass pressure, stiff neck, sensitivity to light, joint and muscle pain, confusion and extreme sleepiness. Public health guidance urges anyone with such symptoms to seek emergency care immediately.
Expert Perspectives and Wider Implications
Trish Mannes, UKHSA regional deputy director for the South East, warned that students can be at risk of missing symptoms because they are easily confused with other illnesses such as a bad cold, flu or even a hangover, and emphasised reassurance that close contacts have been offered antibiotics. A University of Kent spokesperson said the safety of students and staff remains the institution’s highest priority and confirmed close cooperation with public health teams to provide advice and support.
Dr Tom Nutt, chief executive of Meningitis Now, highlighted the rapid progression and devastating impact of invasive meningococcal disease on young people and their families. His perspective underlines why immediate antibiotic administration for close contacts and heightened vigilance for symptoms are core elements of the public health response to this meningitis outbreak.
The human consequence is stark: two people believed to be aged between 18 and 21 have died, and 11 others are seriously ill in hospital. Most of the patients are in the same age bracket and a number are students at the university, a pattern that reflects known vulnerabilities when young people live, study and socialise in close quarters.
Conclusion
The unfolding meningitis outbreak at Canterbury has activated extensive contact tracing, antibiotic distribution and campus-wide communications, but unanswered questions remain about the pathogen’s strain and the full chain of transmission. As investigators continue to interview affected individuals and manage prophylaxis of close contacts, the community faces a tense period of monitoring and care—how will public health teams balance rapid containment with the need for clear, sustained support for students and families?