Mmr Vaccine and the Measles Question: Is the Surge Real or Localised?
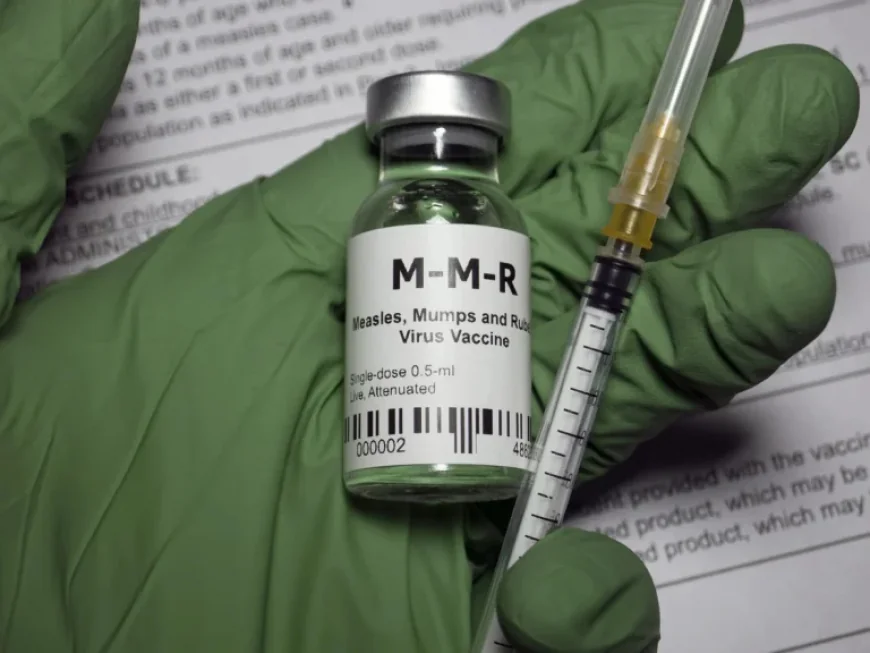
The debate over the mmr vaccine has been rekindled amid clustered measles cases in London boroughs and a wider national narrative of resurgence. While local spikes in Enfield, Haringey and other areas have prompted household warnings, national vaccination coverage and recent case trends paint a more nuanced picture than a simple national epidemic.
Why this matters now
Public concern has intensified because pockets of infection overlap with communities where uptake is lower, and because health bodies have modelled large worst-case scenarios for a major London outbreak. At the same time, national indicators show a fall in confirmed infections from a 2024 spike and steady if reduced vaccine coverage. How policymakers and local services respond determines whether the problem remains local and manageable or escalates.
Deep analysis: what lies beneath the figures
National vaccination rates have edged down but remain well above the crisis low recorded in the early 2000s. Current national coverage stands at about 88. 9 per cent, below the near-93 per cent peak seen in 2013–14 but considerably higher than the sub-80 per cent trough after the early-2000s scare. That long-run context complicates claims of systemic collapse.
Case counts provide a complementary lens. A measurable spike in 2024 produced roughly 2, 900 infections nationwide. The following year, confirmed infections fell sharply to fewer than 1, 000. To date this year the total is 195 confirmed cases; if that pace continued, an extrapolation suggests an annual total below last year’s figure. These patterns point to episodic surges rather than an uncontained national wave.
Yet the national aggregates mask concentrated transmission. London shows clustered infections across at least seven boroughs. Enfield and Haringey account for 95 of the capital’s 146 documented cases, with Enfield alone at 80. The UK Health Security Agency publishes borough-level counts only where ten or more infections are recorded, and it cautions that reported figures are likely to underestimate true infections because of reporting lags. Outside the capital, Birmingham has recorded 43 cases since the start of the year.
Modelling by the UK Health Security Agency offers scenarios ranging from limited local outbreaks to a worst-case London event involving tens of thousands of infections. Crucially, the same modelling makes clear that, based on current evidence, the risk of a widespread national epidemic is low; the models instead anticipate localised outbreaks concentrated where vaccination uptake is weaker, including among certain migrant populations and international travellers.
Expert perspectives
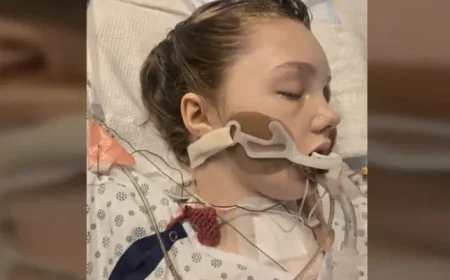
Dr Jo Sauvage, Chief Medical Officer, North Central London Integrated Care Board, emphasises the school-based pattern of spread: “The measles outbreak is mainly affecting children in schools and nurseries, with the most severe cases – requiring hospital treatment – linked to unvaccinated patients. ” She adds that rapid increases in uptake can change the trajectory: “Measles resurges when vaccination rates fall, but this is something we can turn around. The vaccine is safe and effective, and by boosting uptake quickly we can prevent further outbreaks. “
The UK Health Security Agency’s modelling work frames the policy dilemma: while catastrophic scenarios exist on paper, their probability under current vaccination patterns is assessed as low, and the immediate threat is concentrated in communities with low uptake.
Regional implications and ripple effects
The geography of recent cases shifts the locus of response from national alarm to targeted local intervention. In London, a handful of boroughs are the focal points; public-health action there—accelerating routine immunisation in schools and outreach in affected communities—can blunt transmission without invoking sweeping national measures. The contrast between a high national coverage baseline and concentrated local shortfalls suggests resource allocation and communication strategies are the decisive factors.
There are broader governance risks. Framing vaccination as a partisan issue may undermine the civic framing of immunisation programmes and reduce public trust, complicating efforts to raise uptake where it is needed most.
For clinicians and health planners the calculus is clear: preventable severe cases are appearing in unvaccinated people. Rapidly increasing childhood immunisation where coverage has slipped should be the immediate operational priority.
Where will attention fall next: on national panic or on precise, local public-health work to push mmr vaccine uptake back toward previous highs?