Meningococcal Meningitis Outbreak: 13 Cases, 2 Dead After Club Link at Kent University

A meningococcal meningitis outbreak centred on Canterbury has left two people dead and prompted a public-health scramble after some cases attended a nightclub and a university campus. Health authorities have notified hundreds of thousands of people in local networks and are offering antibiotics to identified contacts while specialists work to trace links between the 13 notified cases.
Meningococcal Meningitis Outbreak: Immediate risk and response
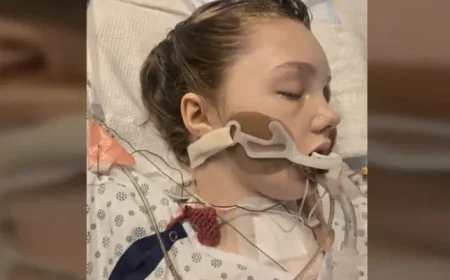
Health officials have notified 13 cases since 13 March, including two people who died. Eleven additional people from the Canterbury area are in hospital and reported to be seriously ill; most of the ill are aged between 18 and 21 and a number are students at the University of Kent. The UK Health Security Agency (UKHSA) is arranging antibiotics for some students in the Canterbury area and has advised that people living and working in certain campus blocks should receive antibiotics without delay.
Why this matters now: links, exposures and community reach
Investigations have identified that some of the cases visited Club Chemistry in Canterbury between 5 and 7 March. UKHSA is asking anyone who attended the club on those dates to come forward for preventative antibiotic treatment as a precautionary measure. Advice has been issued to 16, 000 staff and students at the University of Kent, while the agency is contacting more than 30, 000 students, staff and their families to inform them of the situation and the steps being taken.
Deep analysis: what lies beneath the numbers and immediate implications
The clustering of cases among late-teen and early-twenties individuals and the identified social-event link concentrates risk in settings with close contact. Antibiotics are being deployed as a containment measure for close contacts; specialists are interviewing affected people to map exposure chains and identify who should receive prophylactic treatment. The specific strain involved has not been identified, and that unresolved detail shapes how interventions are prioritised while laboratory work continues. Symptoms associated with meningococcal meningitis and septicaemia can be non-specific early on—fever, headache, rapid breathing, drowsiness, shivering, vomiting and cold hands and feet—while septicaemia can also cause a rash that does not fade under pressure. That clinical ambiguity helps explain why authorities are taking broad precautionary measures among student and community groups.
Expert perspectives and institutional response
Trish Mannes, UKHSA regional deputy director for the South East, warned that students can be at risk of missing symptoms because they are “easily confused with other illnesses such as a bad cold, flu or even a hangover. ” She added that “close contacts of cases have been given antibiotics as a precautionary measure. ” A University of Kent statement said: “The safety of our students and staff remains our highest priority. We are working closely with public health teams and are in touch with staff and students to ensure they get the advice and support they need. “
Regional effects and next steps for containment
The immediate response focuses on targeted antibiotic distribution to those who attended the nightclub on 5–7 March and to students and staff living in identified campus blocks. UKHSA teams are working with the nightclub and university partners to limit further spread while interview-led contact tracing continues. Health messages stress that early medical assessment is essential for anyone developing the listed symptoms, with emergency services advised where conditions worsen.
Where this goes from here
With 13 notified cases, two confirmed deaths and a cluster tied to a social venue and a university, public-health authorities face the twin tasks of arresting transmission and reassuring a large, worried community. How rapidly the specific causative strain is identified, and how effectively close-contact tracing reaches those exposed, will determine whether the outbreak is contained or yields further cases—what patterns will emerge from ongoing interviews and lab results in the coming days?