Colorectal Cancer Deaths Rising in Younger Adults: What a 22-Year-Old Patient Reveals

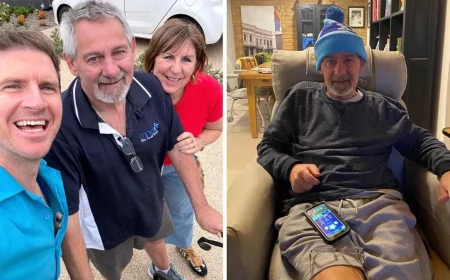
The warning signs of colorectal cancer can look ordinary until they are not. That is the unsettling lesson from a 22-year-old recent graduate whose yearlong stomach pain was first treated as something temporary, then discovered to be a tumor large enough to nearly block her colon. The case has taken on broader urgency because younger adults are now appearing more often in doctors’ offices with a disease long associated with older patients. The pattern is not only about age; it is increasingly about who is being missed and why.
Why this case is forcing a closer look at colorectal cancer
Dr. Marc Greenwald, chief of colorectal clinical services and surgeon-in-chief at North Shore University Hospital in New York, treated the patient and later wrote a case study on her care. He said the hospital is seeing more people under 45, even as cases fall in older adults. In his view, the most dangerous assumption is that a lack of obvious symptoms means nothing is wrong. The patient had no family history, and her pain had come and gone for about a year before scans finally revealed the tumor.
That matters because early-onset colorectal cancer can be subtle until it is advanced. Greenwald said symptoms may not appear at all, which is why new changes in health should not be dismissed simply because someone is young. The patient’s experience also shows how easily abdominal pain can be attributed to stress or another minor cause, delaying care until the condition becomes harder to ignore.
The education gap behind the rise
A separate study published Thursday in JAMA Oncology gives the broader pattern a sharper outline. Using government data on more than 101, 000 adults ages 25 to 49 who died of colorectal cancer from 1994 through 2023, American Cancer Society researchers found that the rise in deaths over the last 30 years occurred almost entirely among people without a four-year college degree.
Overall, the death rate in that age group rose from about 3 per 100, 000 to about 4 per 100, 000. For people who only finished high school, it increased from 4 to 5. 2 per 100, 000. For those with at least a bachelor’s degree, the rate did not change from 2. 7 per 100, 000. Ahmedin Jemal, the study’s first author, said the findings underline the need for public awareness and for younger adults to heed screening recommendations.
Dr. Paolo Boffetta, a researcher at Stony Brook Cancer Center in New York, said the link was not entirely unexpected, but the new paper was the first national study to clearly show it. The pattern suggests that education is functioning as a marker for a wider set of disadvantages, including lower income, poorer diet, less exercise and reduced access to medical care.
What symptoms should not be ignored
Greenwald said people should seek medical attention when they develop new symptoms, regardless of age. In the study context, the symptom list included blood in stool or rectal bleeding; changes in bowel habits such as diarrhea, constipation or narrowing of stool lasting more than a few days; unintended weight loss; and cramps or abdominal pain. For younger adults, that warning is especially important because there are no screening guidelines for people under 45.
That gap is part of the problem. Colonoscopies are recommended starting at 45, and they can both detect cancer and prevent it by removing polyps or abnormal growths before they turn into tumors. But for people too young for routine screening, any change in health becomes more important to track, especially when symptoms are persistent or worsening. The case of the 22-year-old shows how colorectal cancer can already be well advanced before a diagnosis is made.
Regional and wider impact
The broader impact reaches beyond one hospital or one patient. The American Cancer Society estimates that more than 158, 000 cases of colorectal cancer will be diagnosed in the U. S. this year, and the disease remains the nation’s second leading cancer killer. Deaths among adults younger than 50 make up around 7% of the total, roughly 3, 900. Earlier this year, researchers tied younger-adult colorectal cancer mortality to an annual increase of 1. 1% since 2005, making it the deadliest cancer in that age group.
Scientists do not know what is driving the increase, but risk factors cited in the context include obesity, physical inactivity, a diet high in red or processed meat and low in fruits and vegetables, and a family history of colorectal cancer. The screening age was lowered to 45 in 2021, but the study findings suggest that awareness may need to reach well below that threshold. For colorectal cancer, the question is no longer whether younger adults are affected. It is who is being caught in time, and who is not.