Nhs Medical Supplies Iran War: Why NHS Chief Is ‘Really Worried’ and What Hospitals Face Next

The head of NHS England has said he is “really worried” about nhs medical supplies iran war, warning that the system holds only weeks — and in some cases days — of certain medicines. That stark assessment arrives amid recent price concessions, isolated supply shocks over the past 12–18 months and industry claims that cost spikes are already visible even where physical shortages are not.
Why does this matter right now?
The NHS chief executive’s comments underline a narrow margin for error in the national medicine inventory. He stated that the UK imports 75% of its medicine and that contingency teams are focussing on supply-chain risks. While some products are kept centrally and others locally, perishability and storage costs limit how long large volumes can be held. That combination creates a situation in which short-term disruptions can cascade into immediate local pressures on hospitals and pharmacies.
Nhs Medical Supplies Iran War: the vulnerabilities beneath the headline
The deeper picture comprises three interlocking vulnerabilities grounded in recent observations. First, recent “supply shocks” over the last 12–18 months show the system has experienced unexpected interruptions. Second, price movements are already emerging: the Department of Health and Social Care has issued unprecedented numbers of price concessions to manage surging costs, a mechanism intended to keep deliveries flowing when market prices spike. Third, manufacturing and logistical shifts are altering where and how drugs are produced and moved, with some firms switching production sites and key ingredients becoming scarce, which has pushed up several drug prices.
These dynamics mean that even where medicines are still arriving, the economics of supply are changing — a potential early warning signal. The NHS chief cautioned that stock levels are product-dependent: “a few weeks” of supply for many items, but “days for some products. ” That limited buffer narrows the time available for policymakers and supply managers to respond to worsening conditions tied to the conflict.
Expert perspectives and institutional responses
Jim Mackey, chief executive, NHS England, conveyed concern about the fragility of current stocks and described active contingency planning to identify where risks sit in supply chains. Henry Gregg, chief executive, National Pharmacy Association, said pharmacies are not currently seeing direct shortages linked to the conflict but are witnessing disturbing spikes in prices, which he described as an early indicator of potential challenges.
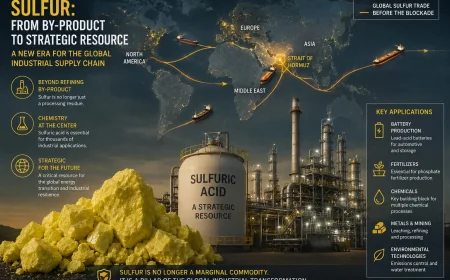
The Department of Health and Social Care’s use of price concessions is a deliberate short-term instrument to keep medicines arriving despite market upheavals. A spokesperson for the Association of the British Pharmaceutical Industry observed that the region is not a significant exporter of medicines and that manufacturers believe supply routes have flexibility to adapt to disruption, but that monitoring will continue. Industry commentary in the context also emphasises that many generic medicines sourced by the NHS from China and India do not transit through the Strait of Hormuz, reducing immediate vulnerability to regional shipping disruptions for those products.
Regional and global consequences for hospitals and patients
The interplay between regional conflict and global manufacturing footprints creates uneven exposure. For branded medicines, commentators note relatively little manufacturing in the conflict zone, so the principal risk is shipping-route disruption rather than production loss. For generics, where production is concentrated elsewhere, the immediate impact of regional naval or shipping disruption may be limited; however, price spikes linked to ingredient shortages or factory transitions can still affect supply and affordability.
Operationally, the NHS and pharmacies are already managing simultaneous pressures: localized shortages of specific items, increasing procurement costs, and the administrative task of applying price concessions to maintain supplies. Hospitals facing higher acquisition costs or intermittent access to specific medicines may need to prioritise use or seek alternatives — actions that carry clinical and budgetary consequences.
Uncertainties remain about how sustained the current pressures will be. The NHS chief’s frank remark that some products may only have days’ worth of stock accentuates the need for rapid, targeted contingency measures that address both logistics and market signals.
As policymakers, clinicians and procurement teams weigh immediate steps, one central question persists: can the combination of central stockholding, price concessions and active supply-chain monitoring avert local disruptions to patient care as pressures tied to the nhs medical supplies iran war persist?